Current evidence on Lipoedema
What is lipoedema?
Lipoedema is a type of fat and connective tissue swelling that predominately affects women, usually triggered around puberty or at times of hormonal change. The aetiology of lipoedema is still unclear, although there is growing evidence of the genetic and epigenetic factors that may influence. In the UK, Grigoriadis et al (2021) investigated clinical characteristics and genetics in 200 women in the UK, identifying genetic influences possibly linked to oestrogen synthesis, lipoma development, and fat metabolism. At present the prevalence of lipoedema remains unknown but is thought to be much more than the 1 in 72,000 previously identified (Child et al 2010). Based on a possible estimate of 0.5-1% of women over 15 being affected by lipoedema, this means that lipoedema may affect up to 22,000 women in Scotland.
Classification of lipoedema
There are various classification systems for lipoedema, but limited evidence. A broad categorisation is given below:
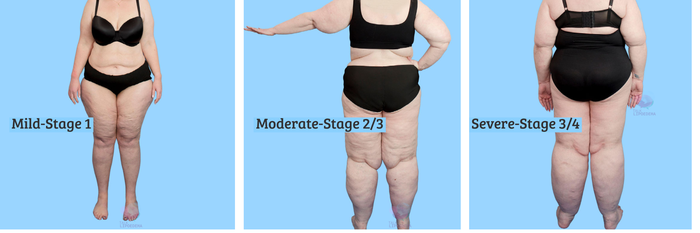
Mild Lipodema or Stage One

'Mild' lipoedema:
- Fat deposition with disproportion between upper and lower body.
- Ankle shape is often lost, but feet are spared.
- Tissues may be sensitive to pressure.
- Bruising or varicosity may be evident.
Moderate Stage Two or Three
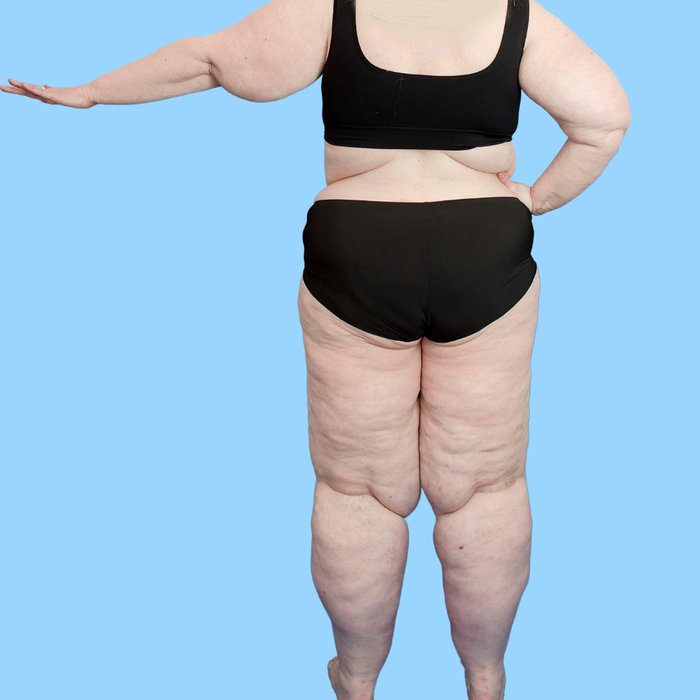
'Moderate' lipoedema:
- Fat lobes are more obvious at the knees and may influence gait.
- Arms and abdomen may be affected.
- Chronic pain may develop
- Problems with hip and/or knee joints.
Severe Stage Three to Four

'Severe' lipoedema:
- Increased weight gain has complicated lipoedema.
- Secondary lymphedema may be present.
- Chronic pain may be more problematic.
- Changes to walking gait.
Pathophysiology of lipoedema
The characteristic pattern of fat deposition leading to distinct shape changes and loss of upper to lower body proportion appears to be due to adipocyte hypertrophy and/or hyperplasia (Wound UK 2017). Commonly, low grade inflammatory processes and tissue hypoxia contribute to chronic pain (Bertsch and Erbacher, 2020). Various studies show increased number of macrophages and pro-inflammatory hormones in tissues, areas of fat necrosis, raised biomarkers indicative of oxidative stress, and increased tissue sodium (Bertsch and Erbacher, 2020; Crescenzi et al., 2018). Hypoxia may also induce the growth of new, fragile capillaries, leading to easy bruising, also seen in people with lipoedema.
There is lack of evidence regarding the potential changes to the lymphatic system in lipoedema. Grigoriadis et al (2021) identified mild pitting oedema in 27% of their participants. It appears that people with lipoedema who experience more progressive generalised weight gain may be more likely to develop secondary lymphoedema (Bertsch and Erbacher, 2020).
References
Alsop, P., Smith, S (2019) Lipoedema: dietary management and dietetic support. Complete Nutrition Focus Vol 11. (3), pp.10-12.
Bertsch, T., Erbacher, G. (2020) Lipoedema: a paradigm shift and consensus. Journal of Wound Care. Consensus Document, Vol. 29 Sup 2. (11) p. 1-53
Child AH, Gordon KD, Sharpe P, Brice G, Ostergaard P, Jeffery S, Mortimer PS. (2010) Lipedema: an inherited condition. Am J Med Genet A. Apr;152A(4), p.970-6.
Crescenzi R, Donahue PMC, Weakley S, Garza M, Donahue MJ, Herbst KL. (2019) Lipedema and Dercum's Disease: A New Application of Bioimpedance. Lymphat Res Biol. Dec;17(6):671-679. [PMC free article: PMC6919257]
Dudek et al. (2021) Quality of life, its factors, and sociodemographic characteristics of Polish women with lipedema. BMC Women’s Health, 21:27 https://doi.org/10.1186/s12905-021-01174-y
Grigoriadis, D., Sackey, E., Riches, K., Zanten, M. van, Brice, G., England, R., Mills, M., Dobbins, S. E., Lipoedema Consortium, G. E. R. C., Jeffery, S., Dong, L., Savage, D. B., Mortimer, P. S., Keeley, V., Pittman, A., Gordon, K., & Ostergaard, P. (2021). [Preprint] Investigation of clinical characteristics and genome associations in the ‘UK Lipoedema’ cohort (p. 2021.06.15.21258988). https://doi.org/10.1101/2021.06.15.21258988
Wounds UK (2017) Best practice guidelines. The management of lipoedema. Wounds UK, London.
For further information on diagnosing lipodema, download our printable sheet for healthcare professionals.
Here is a link to the Best Practice Guidelines in treating lipoedema.
